 A new study offers significant evidence that umbilical cord blood transplants reduce complications after transplant, the need for immunosuppression and the incidence of infections and hospitalizations in leukemia patients. A University of Colorado Cancer Center study released in July 2016 compared outcomes of leukemia patients who had received bone marrow transplants from matched, unrelated donors to those who had received umbilical cord blood transplants between 2009 and 2014.
A new study offers significant evidence that umbilical cord blood transplants reduce complications after transplant, the need for immunosuppression and the incidence of infections and hospitalizations in leukemia patients. A University of Colorado Cancer Center study released in July 2016 compared outcomes of leukemia patients who had received bone marrow transplants from matched, unrelated donors to those who had received umbilical cord blood transplants between 2009 and 2014.
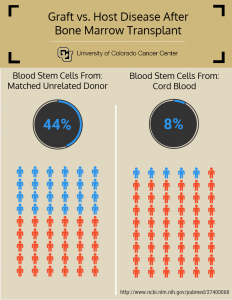
The study examined patients who were at least three years post-transplant and focused on the incidence of graft-versus-host disease (GVHD), a common, potentially fatal complication in transplant recipients. Among the study participants, the incidence of severe graft-versus-host disease was 44% in patients who had received bone marrow transplants from matched, unrelated donors. In comparison, the incidence of GVHD among patients who had received umbilical cord blood transplants was just 8%. In addition, patients who had received cord blood transplants were less likely to require continuing immunosuppression therapy, and had fewer infections and hospitalizations following treatment.
Stem cell treatments hold the most promise for patients with blood cancers after remission is achieved with chemotherapy. The first choice among treating physicians has been the use of marrow from matched, related donors, followed by the use of cells from matched, unrelated donors. Umbilical cord blood and haploidentical transplants have also emerged as promising leukemic therapies.
Currently, donor matching is thought to provide the best chance to avoid complications post-transplant, however the University of Colorado Cancer Center study may change clinicians’ minds about the value of cord blood transplants. In addition to avoiding severe cases of GVHD, cord blood transplant patients experienced a lower incidence of less severe cases of GVHD – 32% compared to 68% among matched, unrelated donor recipients.
A second major post-transplant benefit emerged among patients who received cord blood transplants. Those patients were able to cease immunosuppression therapy safely after a median of 268 days post-transplant. Comparatively, patients who received matched, unrelated donor cells were unable to discontinue immunosuppression therapy in any meaningful way.
Further, new information from researchers at the Fred Hutchinson Cancer Center suggests that leukemia patients at a higher risk of relapse post-transplant fared better when they received cord blood transplants than when they received cells from matched, unrelated donors.
Patients in the Hutchinson study had cancers that were not entirely in remission prior to transplant. Typically, these patients have a one-in-three survival rate three years post-transplant. Patients in the Hutchinson study with minimal residual disease showed a lower relapse rate and better three-year survival rates than patients with minimal residual disease who received matched, unrelated donor cells.
Based on outcomes, the studies may encourage clinicians to re-evaluate their preference for cord blood transplants when a matched, related donor is not available. Typically, all leukemia patients have a 25% chance of finding a matched, related donor, and Caucasian patients have a 70% chance of finding a matched unrelated donor.
Finding matched, unrelated donors is significantly more complicated and less likely among patients of other ethnic backgrounds or mixed ethnicity. Unrelated donors are normally found among people who have previously agreed to donate marrow. That system relies on individuals who volunteer to be evaluated as donor candidates, and who meet all other age and health requirements. Cord blood largely avoids the issue of donor matching because it represents a rich source of immature leukemic cells where HLA matching is not so critical.
These developments underscore the importance of cord blood banking and the promising role of cord blood in the treatment of diseases. If you would like more information about the cord blood banking services available through New England Cord Blood Bank, please contact us at (888) 700-2673.